August 9, 2016
Shared Challenges: Lack of Health Insurance and Quality Care
Too many African-American and immigrant Virginians are locked out of health insurance due to decisions by Virginia’s legislature. Virginia lawmakers have made a number of choices to limit access to health insurance, including in some cases where the federal government would cover all the cost. By not closing the health care coverage gap, policymakers have left 230,000 Virginians without insurance. On top of that, Virginia places additional barriers – above-and-beyond the five-year waiting period that federal law requires – for lawfully present immigrants before they can obtain health insurance through the state’s meager Medicaid.
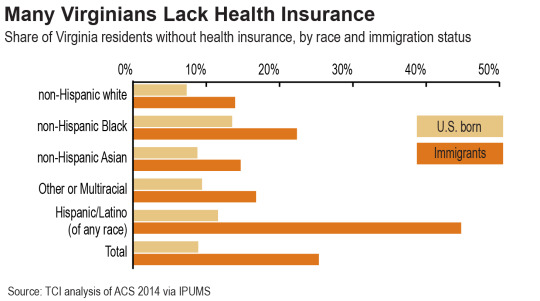
Immigrant Virginians and Virginians of color, especially African-Americans, are much more likely than U.S. born white Virginians to lack health insurance. Just 7 percent of U.S. born non-Hispanic white Virginians are without any health insurance coverage, compared to 14 percent of Virginians who identify as Black or African-American, including 22 percent of Black immigrants living in Virginia. Hispanic or Latino Virginians are even less likely to have health insurance – almost half of all Hispanic or Latino immigrants in Virginia have none. Access to insurance is somewhat better for non-Hispanic white and Asian immigrants, but in all cases immigrants have lower rates of health insurance than is typical for U.S. born Virginians. All told, a majority of Virginia’s uninsured residents are people of color.
And for those who have insurance or can afford care out of pocket, there are often barriers related to the lack of culturally and linguistically competent care. This is a national problem, and while educational institutions for the health field are now incorporating some training in cultural competency, Virginia is not among states that mandates this training as part of continuing medical education.
This lack of cultural competency can lead to unequal care. National research shows that racial minorities face disparities in everything from the use of cardiac diagnostic procedures to the prescribing of pain relievers, even after controlling for socioeconomic status, whether the patient had insurance, and other health factors. African-American, Asian-American, and Latino patients are more likely than white patients to report that their medical provider judged them unfairly or treated them with disrespect based on race or ethnicity and are also more likely to report unfair or disrespectful treatment based on how well they spoke English.
So, what can Virginia do?
Virginia could go a long way toward fixing Virginia’s health insurance gaps that hit immigrants, African-Americans, and Latinos by fixing Virginia’s deliberate barriers to health insurance. This should start with closing the coverage gap by expanding Medicaid and, as an important corollary, making sure immigrant Virginians have a decent shot at qualifying for the coverage by removing the state’s extra barriers on Medicaid access for immigrants that go beyond federal requirements.
In addition to removing legal barriers to public health insurance, Virginia should make sure everyone who is eligible knows about these programs and is able to enroll. This must include enhanced outreach efforts targeting under-enrolled communities and providing program information and registration forms in a variety of languages.
Furthermore, policymakers can make sure Virginia’s public medical and allied health schools are providing clinically relevant cultural information. Virginia can also consider including either a requirement that medical professionals take courses in cultural competency as part of their continuing education work or requiring that all continuing education courses include some clinically relevant cultural and linguistic information.
Virginia should be a leader in providing access to appropriate care for all patients, not just those who are lucky enough to have health insurance and who share the cultural norms and language of their doctors and nurses.
This is the fifth in a series of blog posts based on The Commonwealth Institute’s new report, We’re In This Together: African-American and Immigrant Communities Share Challenges, Policy Solutions. During July and August, we are highlighting analysis and policy ideas from each section of the report. For more information about this report and its findings, please contact Laura Goren at laura@thecommonwealthinstitute.org.
Category:
Immigration
