January 30, 2017
Studied to Death: Virginia Lawmakers Have An Opportunity to Make Real Progress on Mental Health Reform. Will They?
The Virginia Tech shooting in 2007. The tragedy with the son of Senator Creigh Deeds in 2013. The recent death of Jamycheal Mitchell in Hampton Roads Regional Jail in 2016. These tragedies have all added additional layers of urgency to the need to transform Virginia’s broken mental health system. Yet, when it comes to stepping up to fund the changes necessary to improve it and work to prevent future crises, few meaningful steps have been taken at the legislative level. The state has a long history of inconsistent responses to mental health needs, and, over time, this has resulted in an erosion in its national standing for mental health outcomes and delivery of services. This legislative session there are multiple proposals on the table that could improve Virginia’s trajectory.
Today, from a national stand-point, Virginia is recognized as having a mental health system with results well below the national average. Mental Health America ranks Virginia 45th out of all states for mental health services and outcomes for youth, and 38th overall. Despite being a top 10 state for median household income, Virginia is stingy when it comes to mental health spending, ranking 31st in per capita expenditure out of all states.
Virginia has, however, done a good job studying its mental health system in recent decades. In fact, there have been at least 250 state-sponsored studies relating to the mental health system since 1970 that have been presented to the General Assembly. Major reports commissioned since 1970 have largely come to similar conclusions: the commonwealth’s mental health system has serious gaps and requires more funding to improve services and outcomes.
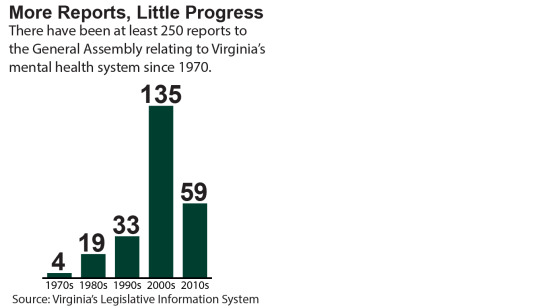
We Know What it Takes to Improve
Many of the reports have hit on similar themes. In 1971, the Hirst Commission found that just 66 percent of Virginians had access to some community-based mental health services, with much more limited access in rural localities. In 1979, the Joint Legislative Audit and Review Commission produced a report calling for better coordination between state institutions and community services, and to develop alternatives to hospitalization. In the 1980s, the Bagley and Emick Commission reports had similar findings, citing a lack of coordination between state and local systems. In 1997, a report chaired by Delegate Ann Rhodes once again found a similar misalignment in coordination, and that community service boards only received 26.6 percent of the state’s mental health funding despite serving 93.9 percent of all patients with mental health needs. Reports in the 2000s had similar findings that the state was inadequately funding mental health services, particularly community service boards.
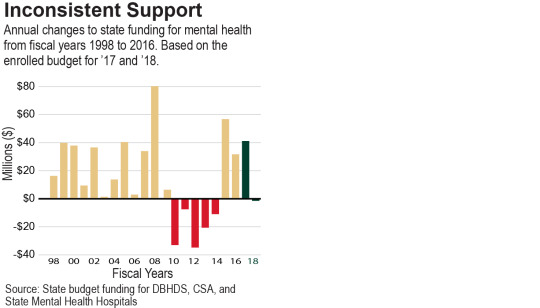
Responding to the recommendations from these studies would require consistent and sustained support from the state. And looking at the changes to mental health spending over the past decade, Virginia has had an inconsistent record. For example, one year after the 2007 Virginia Tech shooting, the legislature committed $42 million over the 2009 and 2010 biennium to expand community-based mental health services throughout the commonwealth. However, most of this funding was quickly rescinded when the recession hit.
Virginia’s current commission studying mental health, the Joint Subcommittee to Study Mental Health Services in the Commonwealth in the 21st Century, has outlined the most recent cost estimates to modernize the state’s mental health system. Meeting the subcommittee’s mission of providing “consistent access to the full array of comprehensive, high-quality mental health services to individuals of all ages regardless of their geographic location or their ability to pay,” would cost around $184 million, with many of the costs recurring on a yearly basis.
Of course, some of the subcommittee’s recommendations could result in cost savings that eventually offset some of these costs. Two of the subcommittee’s top priorities are same day access to care, placing a greater focus on early treatment rather than responding to a more severe crisis later on, and making primary care screenings widely available, in order to identify issues at the outset. This type of care often prevents crises down the line, which are almost always more expensive to treat.
Preventive care can also protect individuals from falling into – or back into – the criminal justice system. Around a quarter of inmates in Virginia suffered from at least one mental health condition in 2014, up 39 percent since 2008. Improved mental health screenings and services offered at the community level throughout the state would keep many of these individuals out of the criminal justice system in the first place, ultimately preventing the much higher price of incarceration.
The governor has proposed funding for the subcommittee’s most urgent recommendations. His recent proposed budget amendments included an increase in mental health and substance abuse funding of $27.2 million for the upcoming budget biennium for programs and services as well as $4.5 million for another study.
Some legislators are also looking to improve mental health services. Two companion bills up for consideration during this legislative session, HB 1549 filed by Delegate Farrell and SB 1005 filed by Senator Hanger, call for community service boards to expand the number of services they are required provide. These services could go a long way to improve mental health outcomes at the community level throughout the state, and funding for them is included in the governor’s budget proposal.
Already during this legislative session, when the Secretary of Health presented the governor’s proposal, which included $4.5 million to hire an independent contractor to study and redesign the state’s delivery system, some legislators responded by calling for even more studies to further look into mental health needs across the state, despite the long list of studies that have already been conducted. The implications from this suggestion indicate that the legislature might not be ready to meet the modest request by the governor to start modernizing the state’s mental health system.
At this point, Virginia has gone through the process to develop solid, well researched steps to move forward in modernizing its mental health system. What continues to be missing is the political will to actually solve the identified problems.
Both Farrell’s and Hanger’s bills go a long way to modernize the state’s mental health system. However, the question now remains whether legislators and the governor will muster the political courage necessary this session and beyond to make the sustained financial commitment necessary to modernize the state’s mental health system and prevent future tragedies.
Category:
Health Care
