April 23, 2020
The COVID-19 Divide: Virus Sheds Light on Inequity
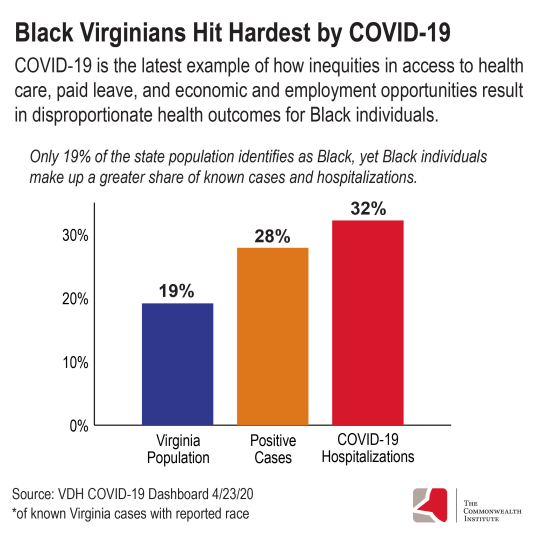
As we navigate the public health crisis, every policy and funding decision made should move Virginia closer to becoming a place where everyone has the opportunity to thrive. On April 8, Gov. Northam announced a commitment to collect better COVID-19 related data by race. Collecting better data will be important to document how different communities across Virginia are being impacted by the pandemic and arm state officials with information needed to target testing and assistance. Unfortunately, the data will likely reinforce what many already know: the effects of structural and historical racism have led to a disproportionate impact of COVID-19 on communities of color. As of April 23, Black Virginians make up 28% of confirmed COVID-19 cases where race was reported and 32% of all COVID-19 related hospitalizations even though only 19% of the state population identifies as Black.
These statistics are enough to raise major concerns but still present a very incomplete picture of the impact COVID-19 has had on communities of color. About one-third (32.8%) of all confirmed cases in Virginia do not have a reported race, so the impact on Black and other communities of color is likely understated given current data trends. These disproportionate outcomes for people of color cannot be addressed with a single policy solution – there’s a need for substantial societal change. Fortunately, state leaders have many policy solutions at hand to address the consequences of past choices and give everyone in the commonwealth a chance at a healthier, more prosperous future.
Disparities Are At Core of COVID-19 Data
National and state leaders have asked people to take precautions such as physical distancing in order to keep themselves and their loved ones safe during this time. However, the ability to self-isolate or to stay at home has been impossible for some and largely unavailable to 80% of Black and 84% of Latinx workers who report not being able to do their jobs remotely. This means many families need to decide between earning a paycheck or putting themselves at elevated risk of contracting COVID-19. Having the funds to pay for essentials like groceries likely takes precedence even if an individual or a loved one has underlying health concerns that can lead to complications with COVID-19. The inability to work remotely may also mean that non-essential jobs are vulnerable in industries hardest hit by COVID-19 such as accommodation and food services – likely leading to layoffs and furloughs that disproportionately impact people of color.
Black communities are contracting COVID-19 at high rates, and this can at least be partially attributed to the fact that many Black Virginians work in industries that have been deemed essential such as grocery stores, public transit, waste management, home health care, and nursing homes. In fact, more than 4 in 10 workers in essential industries in Virginia are Black, Latinx, Asian American/Pacific Islander, or some category other than white. Further, almost a third of all workers in essential industries are Black. As a result, Black workers in the state are truly the front-line workers during this pandemic.
The potential exposure to the virus is compounded when taking into account that only 31% of the lowest wage workers have access to any sick leave. While the federal government has stepped in to ensure sick leave for many, workers in large (500 employees) and small (under 50 employees) companies can be exempt from providing sick leave to its workers.
The confidence to seek health care when feeling symptoms may be dampened by distrust of the health care industry, difficulty navigating the system, language barriers, fear of immigration enforcement for undocumented families and worry about out-of-pocket costs due to being uninsured. In addition to increasing the likelihood of negative health outcomes for patients, these experiences and ongoing concerns create a barrier to accessing timely and regular health care. Roughly 12% of all non-elderly adults are uninsured in Virginia. Yet when you look at uninsured rates broken out by race, we see that 32% of Latinx adults, 16% of American Indian adults, 15% of Black adults, 12% of adults identified as mixed race or “other” race, 9% of white adults, and 8% of Asian American adults lack health insurance.
Long-standing inequities in health care coverage, ability to take paid sick leave, income and employment opportunities, and access to preventative care mean that people of color often have a greater number of health conditions than their white counterparts. This means that not only are Black communities at higher risk of experiencing severe complications due to the COVID-19 virus – seen by the number of hospitalizations – they have been at higher risk for a multitude of other diseases such as diabetes and high blood pressure and have higher mortality rates when experiencing breast cancer, colorectal cancer, and childbirth. This has been the case for years, yet media coverage of the pandemic has now highlighted the unequal health outcomes experienced by communities of color. It’s also important to note the impact that racism itself has on a person. The accumulated stress of having to constantly face racism and discrimination, often referred to as “weathering,” has been attributed to higher mortality and worse health outcomes for Black individuals.
Lack of Information for Other Communities of Color
Unfortunately, the current race categories being reported by the Virginia Department of Health are inadequate for a state as diverse as Virginia. Race is currently being reported as either, “White, Black, or Other” with no identification of ethnicity. This will result in a substantial gap in understanding how the pandemic is impacting non-Black communities of color in Virginia.
Due to Latinx/Hispanic largely being considered an ethnicity and not a race, on the CDC COVID-19 case report form people who identify as Latinx/Hispanic are made to choose a race and then make their Latinx/Hispanic ethnicity known separately. About two-thirds (64%) of Latinx people in Virginia identify their race as white. This could inflate the infection numbers for the white category and downplay the outsized impacts of COVID-19 on communities of color.
Even in the event that people who identify as Latinx are being counted in the “other” category, this identification lumps Asian American, Pacific Islander, American Indian, Latinx, and other communities into a single group. This will not allow researchers and the general public the opportunity to understand the full scope of COVID-19 and how it has impacted these distinct communities.
Next Steps
The COVID-19 pandemic has and will continue to highlight existing inequities and disparities. Federal and state officials have moved quickly to make sure that income support, paid sick leave, and COVID-19 related health services are accessible to most families. However, Virginia COVID-19 data shows these programs cannot undo years of unequal access to resources, health care, and employment opportunities.
Virginia must consider what can be done now and moving forward to ensure better health outcomes for communities of color:
- Collect more detailed race/ethnicity data in order to be better equipped to respond to the short-term and long-term needs of communities of color impacted by the pandemic.
- Ensure COVID-19 testing is available to low-wage workers outside of working hours and in communities of color.
- Provide anti-racial bias training tools to new volunteer and existing health care providers to help reduce discriminatory health practices when patients seek care.
- Implement mandated minimum sick days and a comprehensive state paid family and medical leave program that would ensure all working people in Virginia have the ability to take time to care for themselves, a loved one, or their child.
- Provide hazard pay for low-wage essential workers so they can better afford to take time off if they are feeling sick and pay for health care and other essential needs. Four in 10 essential workers in Virginia are people of color, many of whom are dealing with elevated levels of exposure to coronavirus.
- Ensure that undocumented communities have access to financial and health related support to navigate the impacts of the pandemic.
- Restore funding to eliminate the “40 quarter” barrier for Medicaid coverage for lawfully present immigrants during the upcoming special legislative session.
This pandemic has laid bare many of the racial inequities that have existed for some time in Virginia, particularly in regard to economic opportunity and access to health care. In order to truly be in this together, lawmakers need to make intentional policy decisions to protect and support people of color both now and in the future as we recover from this crisis and rebuild a commonwealth that works for all of us.
Category:
Health Care

